
The following part of the discussion will focus on assessment techniques and intervention strategies to help patients reduce and recover from their activity intolerance. The patient can maintain regular cardiovascular and respiratory functions during activities.The patient can demonstrate physiological improvements over time.The patient can perform basic activities without excessive exhaustion or loss of energy.The patient can display and use effective energy management/conservation techniques.The patient can provide positive verbal feedback in response to the activity level.The expected outcome of a successful care plan may include: Abnormal blood pressure or heart rate level in response to activity levelĪ proper care plan’s goal or expected outcome is to restore the patient’s ability to perform regular activities healthily without experiencing any signs or symptoms of activity intolerance.Abnormal discomfort or dyspnea during activity.Early signs of fatigue, dizziness, and weakness.An imbalance between oxygen supply and demandĪctivity intolerance includes the following symptoms or signs.Extended bed rest / muscular decline/ immobility.Sedentary lifestyle / deconditioned state.Here is a list of factors that may be related to activity intolerance: Related factors Improper oxygen balance, pain, sleep deprivation, depression, low motivation, and severe stress also lead to activity intolerance.įinally, activity intolerance may result from age-related conditions, especially among elderly patients. It includes medication side effects, extended bed rest, a sedentary lifestyle, and restrictions to healthy activity levels. Numerous factors lead to activity intolerance. It’s a state in which an individual has insufficient physiological or psychological energy to endure or complete necessary or desired daily activities. 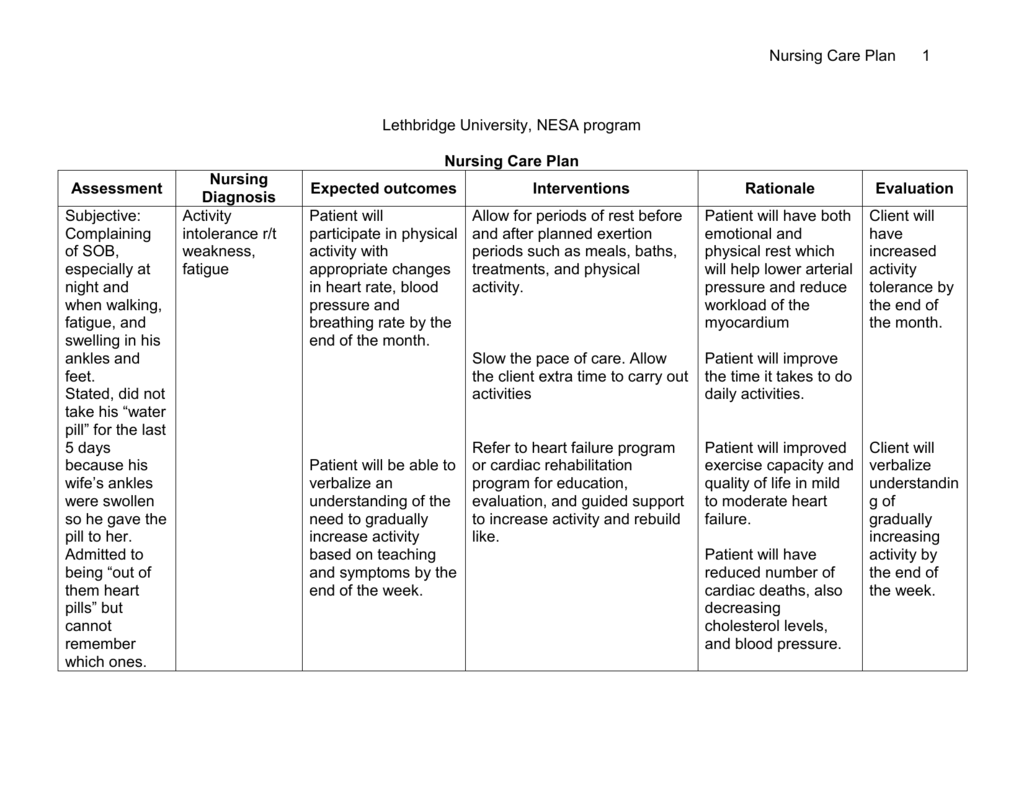 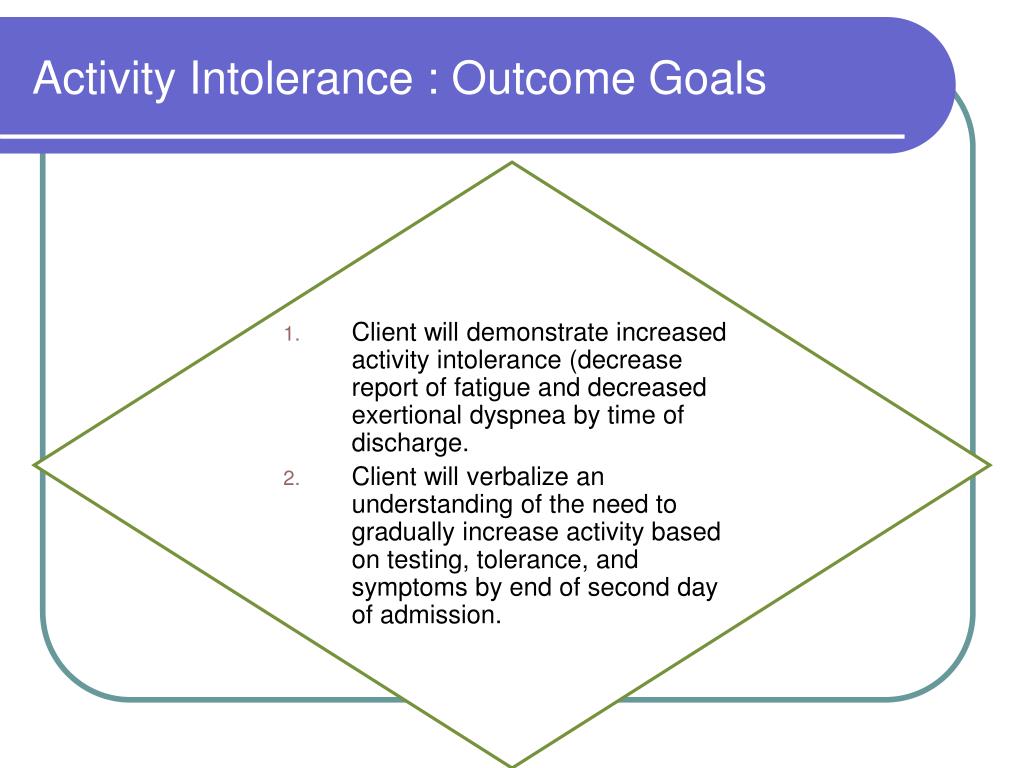
Activity intolerance is a nursing diagnosis defined by NANDA.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
